Hippocrates (400 BC) said “Let thy food be thy medicine and medicine be thy food” and more than two millennia later we are trying to do that.

Hippocrates (400 BC) said “Let thy food be thy medicine and medicine be thy food” and more than two millennia later we are trying to do that.

Like the popular ketogenic diet, Precision Ketogenic Therapy induces nutritional ketosis. However, PKT is a medical therapy – not simply a special diet.
Compared to the typical diet, PKT reduces intake of carbohydrates and replaces those calories with fatty acids. Compared to other ketogenic diets used to treat epilepsy, PKT is more precise in administration and monitoring.
The PKT program process consists of 4 types of appointments, which are accessible by telehealth or in-person clinic visits:
Meal Making and Record Keeping are daily tasks performed by the caregiver.
Click on each appointment or task to learn more.
During the Discuss Keto appointment, a neurologist will evaluate the patient’s need for the PKT Program. The PKT team will explain the PKT Program and the requirements that caregivers must complete daily, as well as answer questions that the caregiver has regarding the program. If the family wishes to pursue PKT, the caregiver will be given orders to complete PKT screening labs.
[ultimate_spacer height=”30″][ult_buttons btn_title=”Learn More” btn_align=”ubtn-center” btn_size=”ubtn-custom” btn_width=”120″ btn_height=”50″ btn_title_color=”rgba(255,255,255,0.49)” btn_bg_color=”rgba(10,10,10,0.35)” icon_size=”32″ btn_icon_pos=”ubtn-sep-icon-at-left” btn_border_style=”solid” btn_color_border=”rgba(15,15,15,0.2)” btn_border_size=”1″ btn_radius=”5″ btn_font_family=”font_family:Open Sans|font_call:Open+Sans|variant:800″ btn_font_style=”font-weight:800;” btn_font_size=”desktop:14px;”]

If the screening labs come back negative, the Pre-Initiation Visit will be scheduled. During the Pre-Initiation appointment, the PKT team will learn more about the patient to create the PKT diet prescription. The PKT team will explain in-depth what the patient and caregiver can expect during the PKT program.
During this appointment, the caregiver can review and sign an informed consent form, which will allow some extra blood to be obtained for metabolomics and a stool sample obtained for microbiomics. The PKT team uses microbiomics data and metabolomics data to understand how to personalize PKT better for each patient and better understand how PKT works.
Patients complete safety labs before initiation and regularly while on PKT.
[ultimate_spacer height=”15″][ult_buttons btn_title=”Learn More” btn_align=”ubtn-center” btn_size=”ubtn-custom” btn_width=”120″ btn_height=”50″ btn_title_color=”rgba(255,255,255,0.49)” btn_bg_color=”rgba(10,10,10,0.35)” icon_size=”32″ btn_icon_pos=”ubtn-sep-icon-at-left” btn_border_style=”solid” btn_color_border=”rgba(15,15,15,0.2)” btn_border_size=”1″ btn_radius=”5″ btn_font_family=”font_family:Open Sans|font_call:Open+Sans|variant:800″ btn_font_style=”font-weight:800;” btn_font_size=”desktop:14px;”]
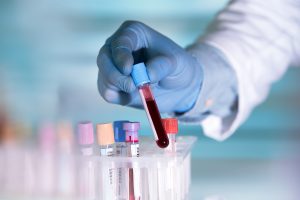
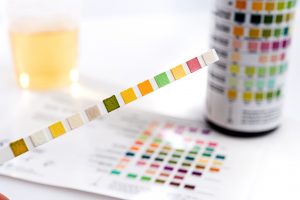
Initiation transitions the patient from usual dietary intake to PKT dietary intake. During this time, caregivers learn how to properly weigh food items, administer supplements, measure urinary ketones, and measure urinary specific gravity. Caregivers also learn how to document home records for daily seizures, daily health status, daily urinary ketones, daily urinary specific gravity, and daily dietary intake.
[ultimate_spacer height=”30″][ult_buttons btn_title=”Learn More” btn_align=”ubtn-center” btn_size=”ubtn-custom” btn_width=”120″ btn_height=”50″ btn_title_color=”rgba(255,255,255,0.49)” btn_bg_color=”rgba(10,10,10,0.35)” icon_size=”32″ btn_icon_pos=”ubtn-sep-icon-at-left” btn_border_style=”solid” btn_color_border=”rgba(15,15,15,0.2)” btn_border_size=”1″ btn_radius=”5″ btn_font_family=”font_family:Open Sans|font_call:Open+Sans|variant:800″ btn_font_style=”font-weight:800;” btn_font_size=”desktop:14px;”]

Monitoring visits ensure that the patient is making progress. These visits can be in-person or by telehealth and will take place regularly.
[ultimate_spacer height=”30″][ult_buttons btn_title=”Learn More” btn_align=”ubtn-center” btn_size=”ubtn-custom” btn_width=”120″ btn_height=”50″ btn_title_color=”rgba(255,255,255,0.49)” btn_bg_color=”rgba(10,10,10,0.35)” icon_size=”32″ btn_icon_pos=”ubtn-sep-icon-at-left” btn_border_style=”solid” btn_color_border=”rgba(15,15,15,0.2)” btn_border_size=”1″ btn_radius=”5″ btn_font_family=”font_family:Open Sans|font_call:Open+Sans|variant:800″ btn_font_style=”font-weight:800;” btn_font_size=”desktop:14px;”]

Meal Making is an ongoing process. The PKT team have several resources for families to make easy to prepare delicious and nutritious PKT meals.
[ultimate_spacer height=”30″][ult_buttons btn_title=”Learn More” btn_align=”ubtn-center” btn_size=”ubtn-custom” btn_width=”120″ btn_height=”50″ btn_title_color=”rgba(255,255,255,0.49)” btn_bg_color=”rgba(10,10,10,0.35)” icon_size=”32″ btn_icon_pos=”ubtn-sep-icon-at-left” btn_border_style=”solid” btn_color_border=”rgba(15,15,15,0.2)” btn_border_size=”1″ btn_radius=”5″ btn_font_family=”font_family:Open Sans|font_call:Open+Sans|variant:800″ btn_font_style=”font-weight:800;” btn_font_size=”desktop:14px;”]

Record keeping is important to ensure patients are thriving throughout their PKT journey. They are critical for fine tuning PKT to give the best result possible.
[ultimate_spacer height=”30″][ult_buttons btn_title=”Learn More” btn_align=”ubtn-center” btn_size=”ubtn-custom” btn_width=”120″ btn_height=”50″ btn_title_color=”rgba(255,255,255,0.49)” btn_bg_color=”rgba(10,10,10,0.35)” icon_size=”32″ btn_icon_pos=”ubtn-sep-icon-at-left” btn_border_style=”solid” btn_color_border=”rgba(15,15,15,0.2)” btn_border_size=”1″ btn_radius=”5″ btn_font_family=”font_family:Open Sans|font_call:Open+Sans|variant:800″ btn_font_style=”font-weight:800;” btn_font_size=”desktop:14px;”]
Each patient receives a PKT cookbook of recipes created specifically for them. Like most recipes, PKT recipes have a list of ingredients and suggested instructions for preparation. Unlike most recipes, PKT recipes require each ingredient to be brand–specific and weighed to the nearest 10th of a gram. Everyone in the PKT village works side by side to create recipes for each patient that are nutritious and enjoyable.
We have prepared recipes that:

PKT can work for all families with the right support. Using PKT therapy can be a big adjustment for any family, but you’re not alone. An interdisciplinary team of health care professionals and researchers unite with families in the PKT Village to make sure that caregivers are successful in making and serving meals at home. This local support is available via telehealth visits so patients and caregivers can have help within the home environment. There are excellent support resources from around the world that are only one click away.

Take a moment to hear from some of our patients’ families what their experience has been like with the University of Florida PKT program.